
Project Mini MEter aims to develop an improved tool/process for measuring infant height.
MIT D-Lab Class
D-Lab: Development Fall 2022
Student team
- Shaida Nishat ‘22 - Shaida studies biology at MIT and hopes to pursue a career in public health focusing on maternal and children's health.
- Shulammite Lim ‘22, M.Eng. ‘23 - Shulammite studies computer science and biology at MIT and plans to become a physician, in which role she hopes to develop thoughtful technologies to address problems in health.
- Elizabeth Ling ‘23 - Elizabeth studies computer science and education at Harvard. She is interested in social impact technology, especially related to health and education.
- Soad Mana, MCP ‘23 - Soad studies city planning where she focuses on community and economic development and data equity. She has engaged in various public health projects in Bolivia and South Africa, where she worked on capacity building projects within local communities.
Community partner
- Turkana Basin Institute (TBI)
- Acacia Leakey, Technical Initiatives Manager
Turkana Basin Institute (TBI) is an international research institute which supports research and education in paleontology, archeology, and geology in the Lake Turkana Basin of Kenya. The three campuses–TBI-Nairobi, TBI-Turkwel, and TBI-Ileret–comprise TBI Kenya, which is under an agreement with the government of Kenya to serve as a repository for the region’s archaeological and paleontological heritage. TBI also runs a mobile clinic, which provides healthcare services to nearby communities.
Location
Northern Kenya
Problem/opportunity
The severe droughts affecting Kenya have led to increased food insecurity and rising rates of child malnourishment and mortality. To combat this, the Turkana Basin Institute, along with the county government and other NGO partners, identifies and provides supplements to malnourished children through its mobile clinic program.1 The mobile clinic measures the children's weight, height and middle upper arm circumference (MUAC) to determine whether they qualify for supplements, but the process of measuring height has proven strenuous. Health workers need to hold the children down against measuring devices, stressing both mother and child and making the work of health workers more difficult. This taxing method provides an opportunity to innovate and improve the mother, child, and health workers' experiences by developing a better measuring tool.
Cultural context
The Turkana Basin Institute field office is located right outside Ileret village, close to the Kenya-Ethiopia border on the east side of Lake Turkana. The main ethnic groups residing in this area consist of the Daasanach, Gabbra, and Rendille communities. These large agro-pastoral communities derive their livelihood largely from livestock and growing maize and sorghum. Some communities, such as the Gabbra and Rendille, are pastoralists who migrate between different areas in the region looking for food for their camel herds.4 However, with sharp economic, political, demographic, and environmental changes in the late 20th century, many former pastoralist families have settled near towns or on farms to pursue agriculture or wage labor. Many pastoralist families have settled in response to drought and famine combined with political violence of livestock raiding and ethnic conflict. A history of isolation and disinvestment in the region has also facilitated rural disparities where communities have limited access to adequate healthcare.
Theory of change
If we develop an improved tool or process for assessing infant health, then community health workers will have access to a better way to go about their routine checks for height measurement. That would improve the healthcare experience for both children and their families, allowing for better relationships between community health workers and community members and encouraging more families to bring their children to the mobile health clinic. This saves time and allows for more children to be served, resulting in reduced malnutrition among children, improved outcomes in children’s education and overall health, and a reduction in the healthcare gap between urban and rural areas. This depends on the community health workers’ willingness and ability to learn and use the new tool, as well as overall stakeholder (e.g., parents, government) buy-in for using a new method. Good metrics for the progress of this project are the accuracy of the measuring tool, the number of community health workers trained on and using the tool, the number of children reached and malnourished children identified, and the time saved when using the tool.
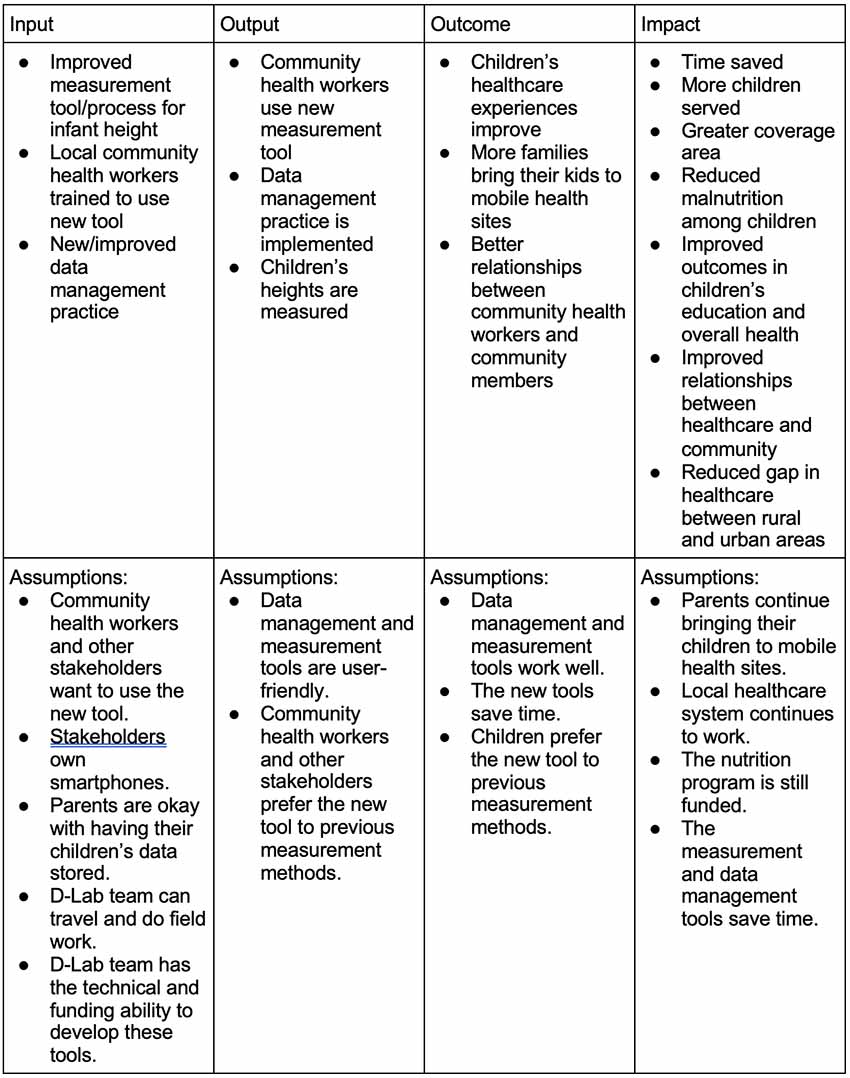
Summary
If we develop an improved tool or process for assessing infant health, then community health workers will have access to a better way to go about their routine checks for height measurement. That would improve the healthcare experience for both children and their families, allowing for better relationships between community health workers and community members and encouraging more families to bring their children to the mobile health clinic. This saves time and allows for more children to be served, resulting in reduced malnutrition among children, improved outcomes in children’s education and overall health, and a reduction in the healthcare gap between urban and rural areas. Good metrics for the progress of this project are the accuracy of the measuring tool, the number of community health workers trained on and using the tool, the number of children reached and malnourished children identified, and the time saved when using the tool.
Potential solution
Our proposed solution is a mobile application that estimates infant height from photos. The application will involve taking a photo of the infant and use augmented reality technology, similar to Apple’s built in Measure app. Users can initially calibrate the application by identifying a few correct measurements with the camera, and health workers would ideally take pictures with similar lighting and position for future uses. Then, the user creates a traced line along the child’s length or height, and the application approximates the line incorporating points in multiple images, focal length of the camera, and inertia while moving.
Next steps
We are working on a method to approximate infant height without lying down, and it remains to see how well the technology works with actual infant positions and camera conditions. Furthermore, there remains the issue of storing and accessing the data, which requires internet access and storage space. While the simplest solution doesn’t store data at all, additional field data can improve the measuring algorithm, but accessing large datasets through the internet may be spotty in remote areas.
In Kenya, we will spend time laying the groundwork for our project. We will visit TBI-Nairobi and TBI-Turkwel, where we will gather information about the project context through observation and informational interviews. We will also brainstorm ideas with TBI staff and community health workers.
References
- More than 1 million children affected by drought in Kenya. UNICEF. Retrieved November 13, 2022, from https://www.unicef.org/press-releases/more-1-million-children-affected-drought-kenya
- Little, Peter D., Hussein Mahmoud, and D. Layne Coppock. "When deserts flood: risk management and climatic processes among East African pastoralists." Climate Research 19.2 (2001): 149-159.
- McPeak, John G. and Peter D. Little. “Pastoral livestock marketing in Eastern Africa: research and policy challenges.” (2006).
- Fratkin, Elliot, et al. “Pastoral Sedentarization and Its Effects on Children’s Diet, Health, and Growth among Rendille of Northern Kenya.” Human Ecology, vol. 32, no. 5, 2004, pp. 531–59. JSTOR, http://www.jstor.org/stable/4603538.
- Galaty, John. "Boundary-Making and Pastoral Conflict along the Kenyan–Ethiopian Borderlands." African Studies Review 59.1 (2016): 97-122. Print.
Contact
Libby Hsu, Lecturer; MIT D-Lab Associate Director of Academics









































